
The food pyramid just got flipped: what the new nutrition guidelines mean for you
Earlier this month, the United States released its Dietary Guidelines for Americans, 2025–2030… and yes, they’ve made waves. The headline message is blunt: eat real food, and stop living on “highly processed foods laden with refined carbohydrates, added sugars… and chemical additives.”
Hallelujah!
Even if you don’t live in the US, these guidelines matter because they shape food policy, product formulation, and public messaging far beyond American borders.
What I hope to achieve with this post is:
- zoom out so you can see how we got here,
- explain the scientific and industry missteps that shaped modern eating, and
- translate the new recommendations for you into practical, real-life action, through the lens of low-carb Mediterranean living, which remains a sustainable and delicious eating pattern that’s appropriate for everyone.
How we got here: a quick (and important) history
If we go back to the 1960’s and 1970’s… there was a great deal of curiosity and scientific investigation around the question of whether what we eat impacts our health. Research was focused on finding the cause of heart disease. The fear of heart attacks and strokes is what shaped modern dietary advice.
A key milestone was the 1977 “Dietary Goals for the United States” report, which promoted reducing total fat and saturated fat, and emphasised carbohydrate intake (often framed as “complex carbohydrates”).
Then, in 1980, the US began issuing the Dietary Guidelines for Americans every five years. Over time, the messaging increasingly leaned toward low-fat eating.
By the early 1990s, the classic food pyramid era reinforced the idea that fat was the problem and that every meal should be based on carbohydrates (specifically grains).
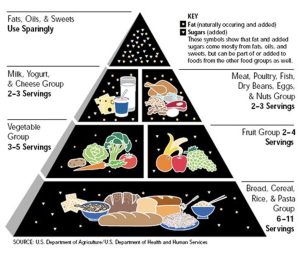
When I was at medical school in the early 2000’s, we had 1 lecture on nutrition and my foundational nutrition knowledge that I imparted to many patients in my early career was fundamentally flawed.
To be fair, the intention was not evil, it was to reduce cardiovascular risk. But several things were true at once:
- Nutrition science at population level is hard. Much early guidance relied heavily on observational data, surrogate markers, and imperfect dietary reporting. (A problem that continues today.) It’s really difficult to get an accurate idea of what people eat… and even more challenging to consistently get people to eat a particular way so you can study the effects of diet on health.
- “Reduce fat” got simplified into “all fat is bad,” without enough distinction between ultra-processed fats and whole-food, naturally-occurring, healthy fats. Cholesterol in food was demonised because the assumption was that dietary cholesterol caused high blood cholesterol, and high blood cholesterol leads to blocked arteries.
- The food environment responded faster than the science: “low fat” became a marketing label, to promote sales and increase profits under the guise that “low fat” = “good for you”.
The unintended consequence: “low-fat” became “highly processed”
When you remove fat from food, you remove flavour and satiety. The food industry solution was predictable: add sugar, refined starches, flavourings, and clever chemistry. Make food products that are palatable, cheap to produce and market them as “low-fat” because the government scientists say that’s the way to prevent heart disease.
A major shift was the introduction of high-fructose corn syrup (HFCS) in the food supply and soft drinks during the 1980s. This cheap, powerful sweetener was added to almost everything to enhance flavour, but also to make people eat more. Adding any form of sugar increases appetite, decreases satiety signalling and triggers dopamine release – making processed foods highly addictive.
Alongside these changes, obesity rates rose dramatically over the following decades (for example, US adult obesity increased from about 15% in 1976–1980 to around 34% by 2007–2008).
Now, to be clear: one policy didn’t “cause” the entire metabolic health crisis. Physical inactivity, portion sizes, hyper-palatable convenience foods, sleep disruption, stress, alcohol, and socioeconomic factors all play important roles. But the direction of the messaging (“avoid fat”) made it far easier for a processed, sugar-rich food system to thrive.
What’s new in the 2025–2030 guidelines?

The new document is short (10 pages) and very direct. Here are the big shifts:
1) “Prioritise protein” — with a much higher target
They recommend 1.2–1.6 g of protein per kilogram of body weight per day.
They also explicitly include red meat as a healthy option (along with eggs, poultry, seafood, legumes, nuts, seeds, soy products).
2) Full-fat dairy is back
They advise full-fat / full-cream dairy with no added sugars, and quote 3 servings/day for adults.
3) A stronger stance on ultra-processed foods and sugar
They say to avoid highly processed salty/sweet foods and avoid sugar-sweetened beverages. They also state that no amount of added sugars or non-nutritive sweeteners is recommended, and give a practical cap: no more than 10 g added sugar per meal.
4) Whole grains are de-emphasised (but not removed)
They recommend 2–4 servings of whole grains per day (which is much less than the 6-11 servings suggested in the previous food pyramid), while consciously “reducing refined carbohydrates.”
5) Fats: “whole-food fats” are encouraged — but saturated fat caution remains
They promote fats from whole foods and name olive oil as a preferred cooking fat, while also listing butter and beef tallow as options.
At the same time, they keep the long-standing guideline that saturated fat should generally stay under 10% of total daily calories, and they explicitly say more high-quality research is needed on which fats best support long-term health.
6) Gut health gets a spotlight
They mention the microbiome and encourage vegetables, fruits, fermented foods, and high-fibre foods, while warning that highly processed foods can disrupt this balance.
My take: how this fits (and doesn’t fit) with my nutrition philosophy (low-carb Mediterranean living)
There’s a lot here that I genuinely like:
- The strongest message is no longer “avoid fat.” It’s stop eating food-like products, and eat real food instead.
- The hard line on sugary drinks + added sugars is a win for metabolic health.
- The focus on protein will help many people with satiety, muscle maintenance, and healthier body composition.
But from a low-carb Mediterranean perspective, I’d add two practical “filters”:
Filter 1: Protein quality and context matter
Yes, to protein! But choose un-processed free-range / grass-fed options. For my patients, I see best results when protein is paired with:
- lots of non-starchy vegetables
- olive oil, olives, nuts, seeds, avocado
- frequent fish/seafood
- and sensible portions of legumes (depending on personal tolerance and metabolism)
Filter 2: Don’t stress about saturated fat intake, if the source of fat is healthy and real
The guidelines still advise staying under 10% of calories from saturated fat. But, this can be tricky if you are including healthy, natural fats from grass-fed meat, chicken with the skin on, eggs, full-cream dairy products, and coconut.
Mediterranean rule of thumb: let extra virgin olive oil be your default fat, use butter, cream and tallow when you want extra flavour (occasionally), and use fish, nuts, seeds, avocado as additional regular healthy fat sources.
What the new guidelines practically mean for you
Here’s a very usable way to apply the 2025–2030 guidance without getting lost in ideology:
1) Build meals around: protein-based foods + plants + healthy fat
- Protein: eggs, fish, chicken/poultry, Greek yoghurt, tofu/tempeh, lentils/beans, good-quality meat
- Plants: 2–3 handfuls of colourful veg per meal (fresh/frozen/canned with minimal additives). Try to eat a wide variety of different plants.
- Fat: use olive oil, olives, avocado, nuts/seeds as your day-to-day sources of healthy fats. Artisanal cheeses, butter and cream are allowed.
2) Make carbohydrates intentional, not automatic
The new guideline recommends 2–4 servings of whole grains/day, but you don’t have to include carbs, especially if you’re insulin resistant or trying to lose weight.
A low-carb Mediterranean approach often works beautifully with:
- carbs mainly from veg, berries, legumes in modest portions, and infrequent small servings of whole grains.
3) Avoid added sugar
If you want an easy “line in the sand,” borrow their meal rule: ≤10 g added sugar per meal. I usually advise <5g sugar per 100g of any food product you are planning to buy.
Remember to read the label! That one number can change your shopping trolley fast.
4) Swap “processed convenience” for “real convenience”
You don’t need to cook like a chef. You need easy, quick and healthy defaults:
- rotisserie chicken + salad + olive oil
- tinned tuna/sardines + cucumber/tomatoes + feta
- eggs + frozen veg + herbs/spices
- bean stew + cottage cheese + salad
5) Add one gut-friendly habit per day
They explicitly encourage fermented foods like kefir, kimchi, sauerkraut, miso.
Pick one that fits your culture and taste, and make it routine.
A simple “day of eating” (low-carb Mediterranean style)
- Breakfast (optional): Greek yoghurt (unsweetened) + berries + walnuts + chia seeds + cinnamon
- Lunch: Big salad (greens + tomatoes + peppers + cucumber + olives + avo) + grilled chicken/tuna + olive oil + lemon juice
- Dinner: Salmon (or lentil/bean stew) + roasted vegetables + olive oil dressing
- Snack (if needed): cheese + apple OR boiled eggs OR nuts
This aligns with the new “real food” framework while keeping carbs controlled and nutrient density high.
The bottom line
After decades of public messaging that often drifted into “fat is the enemy,” the newest guidelines swing the spotlight back where it belongs: real food, fewer refined carbs, far less sugar, and less ultra-processed eating.
If you want the simplest action plan:
- Protein at each meal,
- vegetables everywhere,
- olive oil as your default fat,
- cut sugar and sugar-sweetened drinks,
- shop the perimeter of your supermarket, and
- treat packaged foods as “sometimes,” not “daily.”
